You want a straight answer about mammograms. Instead, you get a shouting match between medical boards.
One doctor tells you to start at age 40. Another says 50 is fine. One guideline says get scanned every single year. Another insists every two years is safer. It feels like gaslighting. Breast cancer is terrifying, and the medical establishment cannot even agree on when to look for it. Learn more on a similar topic: this related article.
The confusion stems from a fundamental disagreement on how to balance saving lives against causing medical harm. Screening is not a free pass. It comes with a price tag of anxiety, false alarms, and overdiagnosis. To make the right choice, you need to understand the math, the mechanics, and the actual risks.
The Real Reason Medical Groups Argue Over Your Breasts
The data pool is the same for everyone. Every major medical organization looks at the same clinical trials, the same mortality rates, and the same statistics. Yet, they reach completely different conclusions. Additional reporting by National Institutes of Health explores comparable views on this issue.
This happens because different organizations prioritize different outcomes.
Organizations like the American College of Radiology (ACR) and the Society of Breast Imaging look at things through a single lens: saving the maximum number of lives. Their math is simple. Finding cancer early gives you the best chance of survival. Because breast cancer can and does happen in your 40s, they recommend annual mammograms starting exactly at age 40.
On the flip side, groups like the U.S. Preventive Services Task Force (USPSTF) look at public health on a macro scale. They weigh the benefits of a test against the collective harms done to a population. For years, the USPSTF pushed the starting age to 50. Recently, they shifted their official stance, advising women to start biennial screening at age 40. Even with that shift, they still recommend scanning every two years instead of every year.
Why the hesitation? Because mammograms are far from perfect.
The Dark Side of Screening Nobody Wants to Talk About
We are conditioned to think that more testing is always better. In medicine, that is a dangerous assumption. Mammograms carry real risks that have nothing to do with radiation and everything to do with what happens after the scan.
False Alarms and the Spiral of Anxiety
About 10% of women who get a mammogram are called back for more testing. If you have ever received that phone call, you know the absolute terror it causes. Your stomach drops. You spend days or weeks convinced you are dying.
Then you get the diagnostic ultrasound or the needle biopsy, and it turns out to be nothing. A benign cyst. Dense tissue. A shadow. While you might feel relieved, you just endured unnecessary psychological trauma and an invasive procedure.
The Problem of Overdiagnosis
This is the hardest concept for most people to swallow. Not all cancers are killers. Some breast cancers grow so slowly that they would never cause symptoms or shorten your life.
Take Ductal Carcinoma In Situ (DCIS), often called Stage 0 breast cancer. It is confined to the milk ducts. Some DCIS cases will turn into aggressive, invasive cancer. Others will just sit there quietly forever.
The terrifying truth? Pathologists cannot look through a microscope and tell you with 100% certainty which ones will turn deadly and which ones will stay dormant. Because doctors cannot take that risk, almost everyone gets treated. You end up getting surgery, radiation, or chemotherapy for a tumor that never would have hurt you. That is overdiagnosis, and it changes lives for the worse.
Breaking Down the Guidelines by the Numbers
Let's look at what the major players actually recommend so you can see the landscape clearly.
- U.S. Preventive Services Task Force (USPSTF): Start at age 40. Get a mammogram every two years. Stop at age 74.
- American College of Radiology (ACR): Start at age 40. Get a mammogram every single year. Continue as long as you are in good health and have a life expectancy of at least 10 years.
- American Cancer Society (ACS): Start optional screening at 40. Regular mandatory screening should begin at 45. Switch to every two years at age 55, or choose to stick with annual scans.
The gap between these recommendations leaves you stuck in the middle. If you screen every year starting at 40, you maximize your chances of catching an aggressive tumor early. You also double your chances of a false positive over a decade compared to screening every two years.
How to Calculate Your Personal Starting Age
You are not a statistical average. You cannot base your healthcare entirely on a generalized population guideline. Your timeline depends heavily on your specific biology and family history.
The 10-Year Rule for Family History
If your mother, sister, or daughter had breast cancer, the standard rules do not apply to you. The rule of thumb among oncologists is to start screening 10 years earlier than the age your youngest first-degree relative was diagnosed.
If your mother was diagnosed at age 44, your screening journey starts at 34. Period.
The Dense Breast Factor
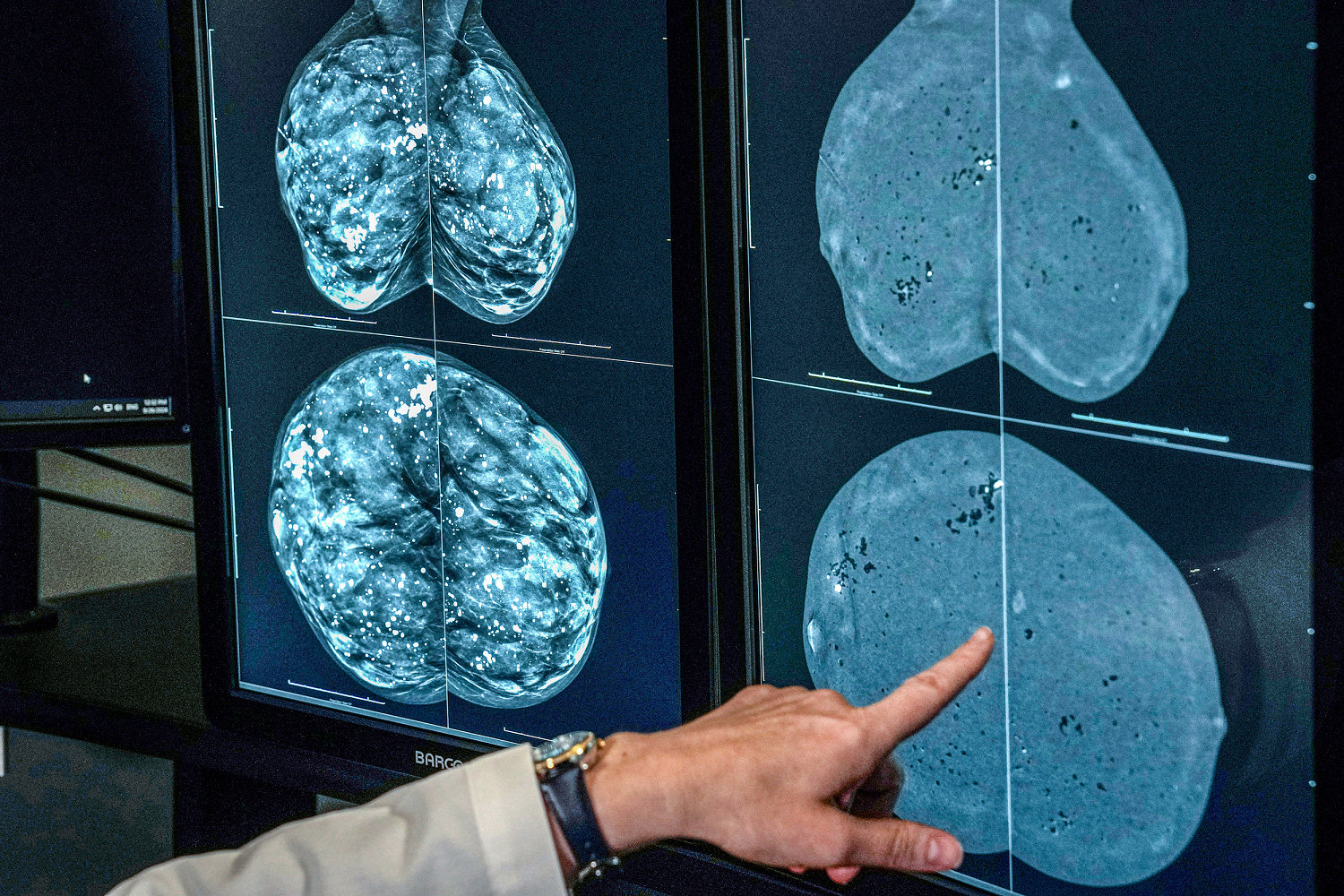
When you get a mammogram, the radiologist looks at the ratio of fat to fibrous tissue. If you have dense breasts, your report will state it. Dense breast tissue looks white on a mammogram. Cancer also looks white.
Trying to find a tumor in a dense breast is like trying to find a polar bear in a blizzard.
If you have dense breasts, a standard 2D or even a 3D mammogram (tomosynthesis) might not be enough. You need to talk to your doctor about supplemental screening, like a breast ultrasound or an MRI.
Genetic Mutations
If you carry a BRCA1 or BRCA2 gene mutation, your lifetime risk of breast cancer skyrockets up to 70%. In this high-risk bucket, screening starts much earlier—often at age 25 to 30—and relies heavily on annual breast MRIs, which are far more sensitive than mammograms.
Your Immediate Next Steps
Stop waiting for the medical community to agree on a single piece of paper. It is not going to happen anytime soon. Take control of your own screening schedule right now.
First, pull up your family medical history. Find out exactly who had breast or ovarian cancer and at what age they were diagnosed. Write those numbers down.
Second, call your primary care doctor or gynecologist and schedule a formal breast cancer risk assessment. Ask them to calculate your lifetime risk score using validated tools like the Tyrer-Cuzick model or the Gail Model.
If your lifetime risk is under 15%, you are at average risk. You can comfortably choose to start at age 40 or 50, choosing annual or biennial scans based on your personal comfort level with anxiety versus early detection. If your risk is above 20%, you are high risk. You need to bypass the standard guidelines entirely, start screening earlier, and get an order for alternating mammograms and MRIs.
Do not let the conflicting headlines paralyze you. Use the discordance as permission to customize a plan that fits your actual life.